
The insurance company’s “explanation of benefits” explains nothing. In fact it often confuses matters more.
Also: People believe their insurance companies are paying more than they really are, because quite often the explanation of benefits leads to that conclusion.
When I founded this company, a major impetus was the fact that people told us they could not understand an “explanation of benefits.” Or a bill. Sometimes it seems that there’s a conscious effort to hide information, just as there is in the old street-con card-hustler game called “three-card monte” (see an example in this Youtube video).
And in fact there is. Discussing the explanation of benefits, an insurance executive told me once, “We make them confusing intentionally, so people can’t understand them.” Anyone who has taken even a passing glance will say that confirms a suspicion: “This is not a bill” and “This page intentionally left blank” and “You may owe your provider” are all common occurrences.
This paperwork is described as “a mismanaged, tangled, screwed-up and incompetent mess,” by Dave deBronkart, a.k.a. ePatient Dave, in this blog post: It takes off from a New York Times piece on the labyrinth of medical bills by Tara Siegel Bernard.
So.
We’ve seen a lot of these, especially in our recent partnership reporting on and crowdsourcing health prices in our award-winning work with partners, investigative reporter and anchor Lee Zurik at WVUE FOX 8 Live and Jed Lipinski and Manuel Torres at NOLA.com I The Times-Picayune, and their teams. To read about this partnership and to see our work, go here; to read about other national partnerships at ClearHealthCosts, go here.
Because we’ve seen a lot of them and can show you the results, without revealing patient’s personal health information but using their shared paperwork to enlighten you, we’re doing this blog post with some examples.
Patterns in the explanations of benefits
They’re very different, but they do show some patterns:
- The numbers don’t look like they make sense. A $498.99 bill, written down to a $13.32 allowable amount? How can that be? Read on.
- Related: Sticker prices are crazy high.
- For an employer or individual insurance policy, the insurer will make a writedown, discount, or adjustment to set it at an “allowed” amount,” “member rate” “contracted amount” or something similar. This contracted amount is agreed upon by the doctor (hospital, lab) and the insurer. This contracted amount is not public: These rates are shrouded in secrecy by gag clauses in contracts between insurers and providers. “Allowed” or contracted amounts can be crazy low, crazy high or in between. Non-private payment rates, Medicare and Medicaid, have payment amounts established by statute. With new transparency laws, hospitals are supposed to reveal their contracted rates, but they do this only sometimes, and the revealed rates are hard to find on a hospital’s site.
- Insurers are paying a lot less than people think they are, and the EOB is designed to perpetuate that confusion. Often the insurer imposes a discount (or writedown or reduction) off the billed price, then adds the “discounted amount” and payment, and puts them on one line. This makes it look like the discount off the contracted rate is part of the payment. Time and again, people assume that the discount and the payment add up to the insurer’s contribution.
- Many insurers don’t identify what procedure actually took place. They often leave out the procedure name and the procedure code, leaving the patient with only a date of service and a provider name. This seems intentionally obfuscatory. Lipinski wrote about this practice at Blue Cross and Blue Shield of Louisiana in this post. We think it’s widespread in the industry — and a way of obscuring what really happened.
- Often the numbers on a bill don’t add up. It seems sometimes that a string of chimpanzees are typing random numbers into a bill.
- Anyone who’s tried to explain or argue a bill with the help of an insurer or a provider knows that hours on the phone in phone-tree and voice-prompt hell, and listening to hold music, are required to even ask a question. Asking the question seldom guarantees a straight answer.
So here are some examples of bills, part of our continuing effort to shed light on billing and explanation of benefits practices.
Get ready for some crazy numbers. This bill for medications shows the extremely high sticker price, marked down immediately to “Allowed,” a fraction of the charged amount. This has several effects: 1) Makes the bill look completely puzzling. 2) Seeks to establish that health costs are really high. 3) Encourages you to believe that your insurance company is a great negotiator, because it’s able to negotiate such a dramatically lower rate. 4) Encourages you to buy more insurance so you can be protected from high prices.

Fairly clear notion of what was done. This bill for a two-part hearing test includes description and also the 5-digit CPT or HCPCS code for both. As is common, the billed amount is routinely written down by the insurer to a “member rate.” Sometimes this is called a “discount,” “contracted rate,” “negotiated rate” or “adjustment” or something similar. (This is a really expensive pair of hearing tests, by the way — they were done at a hospital, which is almost always the most expensive option.) For more on the coding systems that govern billing and payment, go here.

Remicade infusion at a Kaiser facility. Fairly clear what was done — the billing codes are present, with descriptions. But how much was paid? Not at all clear; “Paid by insurance/ Adjustments/ Discount” are all together on one line. Note here that Kaiser is both provider and insurer, so they are essentially billing themselves, and granting an adjustment/discount to themselves, and paying themselves.

The insurer applied a “discount” to the billed price, but did not pay anything. The patient paid the allowable or discounted price in full.

So how much did the insurance company pay? The payments/adjustments total $359.95, but how much was payment and how much was adjustment? The patient thought the insurance company paid the entire sum.

Payments and adjustments clearly broken out. This is clear. Not as common as we might hope. Another bit of good news: Her total amount owed was just $150 on surgery to repair a digit nerve.

Exactly the same thing on exactly the same day? Two abdominal ultrasounds, one transvaginal and one not. And both are billed to her, with the insurer paying nothing. She has polycystic ovary syndrome, so this test must be done regularly, and she was shocked at this year’s bill.

Same patient, same procedure, preceding year: Only one. That time, the plan paid $110.64, and only one was authorized.

A $2,130.90 bill. Insurance “discounts” of $1,432.03. Insurer paid nothing. Patient owes $698.87. The patient thought the insurer paid $1,432.03.

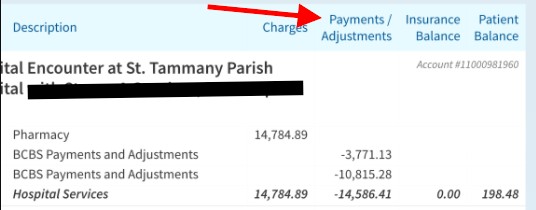
So the payments and adjustments (discounts, or whatever you want to call them) on this colonoscopy totaled $14,586.41. But what did they really pay? Also, it’s a colonoscopy, so how could the charge be labeled “Pharmacy”? By the way, the patient believed, once again, that the insurer had paid the entire $14,586.41.
Crazy emergency room bill. She said the sign said “accepts all insurance.” Sadly, no.

Discounts AND reductions from Blue Cross Blue Shield of Texas on this MRI. So Blue Cross wrote off or discounted $921.38, nearly 50 percent of the charge of $1,997.75. Our database shows you could have this MRI for cash in the New Orleans area from multiple providers for less than half the covered amount. Note “amount covered (allowed)” footnote refers to “the savings we’ve negotiated with your provider for this service.”

The numbers don’t add up: Charge, $307. Contract savings, $147. Insurance paid, $0. Patient paid, $80. But $147+80=$227, not $307. So patient pays $80, twice? And what’s the meaning of the denial code “bundled”? Confusing.

Complete contempt for the idea that the numbers should add up and make sense. What are all these $0 charges, along with payment-adjustment and balance? Transfer from Insurance is charged at $0 and adjusted at $1,200? And the $0 Blue Shield Payment from BS, multiple times? None of this makes any sense at all.


Drug screening test from a pain clinic.

It’s a bill for a brain MRI of $6,349. The insurer approved just $380.23; they paid $201.13, while the insured person paid $175. And what is the mysterious “sequestration” of $4.10″ ? Glad you asked! Look here and here: Automatic, across-the-board spending cuts from 2011. And that blood test — provider billed $98, plan approved nothing, and charged patient nothing. Mysterious.

She said it was an “extracranial study” with a CPT code of 93880. On a bill of $1,171, they paid $238.73. She pays $592.30 in combination of deductible and coinsurance.

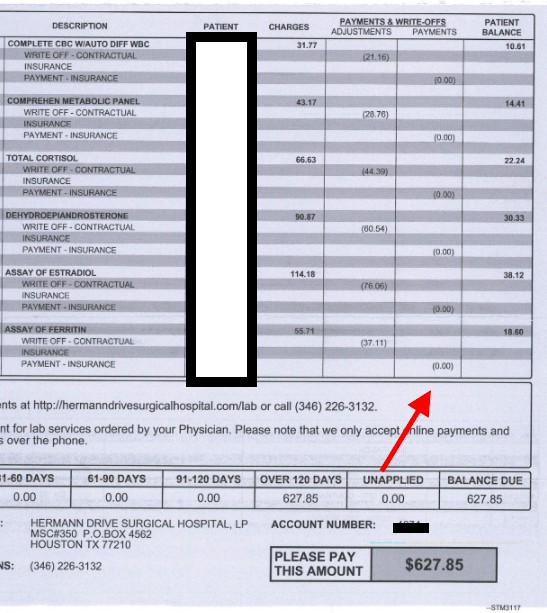
The insurer paid nothing on this long string of blood tests (partial bill). “There was an adjustment because I did have insurance,” she wrote “the adj. of $1252.91 left me with the bill of $627.85. This was part of a physical that is fully paid by the insurance. I did not give permission to do tests that were not part of the covered physical exam but somehow still was billed for this.”

Her note: “I got three stitches.” Bill: $1,124. No insurance discount, no payment, no explanation — just instructions on how to pay.

“I have medical billing experience and even I can’t understand or be certain of some of the things I am billed for,” she wrote. “I know that I had a colonoscopy where 2 benign polyps were removed but I have no idea what the actual CPT code is that was submitted. While I know that a procedure may have many different CPT codes, can’t the insurance company give at least a broad breakdown of these costs so that I can at least attempt to understand if I am being charged for the correct service? Additionally, I know that this charge does not include the charge for the pathology analysis of the polyps that were removed and I’m not entirely sure that the Anesthesiologist charge is included.”


She was billed for four separate colonoscopy procedures. Her insurer paid nothing.

Emergency room charge: $2,130.90. Insurance paid nothing, but applied a $1,432.03 discount. She paid $698.87.

His note says this was a CT scan, not an X-ray. “Outrageous price being reclaimed by Helen Ellis Memorial Hosp (now AdventHealth) in Tarpon Springs, FL.” Note also: Part of his payment was from the deductible, and part was co-insurance – clarifying for us again how it’s not just the high deductibles, but also high co-insurance that is slamming patients.

Gall bladder removal. Of the $10,577.10 charge, Blue Cross discounted $6,214.85 and paid $3,489.85; patient paid $672.46.

“This bill was for a CT scan of the elbow. I recieved a separate bill from the doctor that administered the meds during the CT scan.”

Chest X-ray for $265.78. Compare others here, from $20 to $988.

MRI at Sloan-Kettering. Fairly clear. Billed $5,329.69, plan paid $1,659.01, patient paid $184.33.

The insurer paid nothing. Instead, they just adjusted it down by the $120.38 — the sum is clearly marked as a “contractual adjustment” although the column heading says “Payment/adjustment.”

Allergy test office visit. Charges $411; payment-adjustment together $341 — so what did they actually pay? No way to know.

A discount off a fancifully high sticker price does not necessarily mean you saved money. This procedure, an echocardiogram with Doppler, can be found under $400 on cash at many places in the neighborhood of Clearwater, Fla., where this procedure took place. Here’s a search on our site for cash prices in that locale.

What did the plan actually pay? This emergency room visit shows “Plan Savings,” which is clearly different from “Plan paid.” But what did the plan pay? Nothing? And was the $449.86 applied to the patient’s deductible?

A colonoscopy. The community member told us: “I received a cost estimate from Kaiser of $1,200 for the total cost of the procedure prior to the procedure. They billed the procedure at $16,047.10.” The bill from Kaiser is not illuminating: $9,414.14 is a combination of “Paid by Insurance/Adjustments/Discount” — leaving the patient responsible for $6,632.96. Again, she had no way of telling what they actually paid, but thought it was the $9,414.14.

Sometimes, though, the bills can be pretty clear. Here’s one for an emergency room visit: clearly marking the charge, the discount, the amount due to provider, what the insurer paid and what the individual is responsible for. The fact that it’s clear lets us see that — once the explanation is matched up with the bill — that the patient was asked to pay $278 for a chest X-ray, the only radiology charge here; the insurer allowed $205.72 for that, after plan discount. That chest X-ray can cost $35 or so many places. In hospitals, it’s more expensive.

Read the notes, and compare carefully. This woman had a colonoscopy, and the hospital initially sought to charge her for an anesthesiologist. She refused well before the procedure, so was sure no anesthesiologist had been used. The insurer refused to pay for the non-existent anesthesiologist, saying in its footnotes when that claim was denied that it was part of the “contracted and/or case rate paid to the provider. She was also charged a facility fee, medical services fee and recovery room fee at the same time. The insurer figured her total responsibility for all of this at $1,999, noting that “medical service” and recovery room were part of the facility fee charge. (See first screenshot here.) She asked to be billed properly — so the insurer re-billed, omitting the anesthesiologist but still figuring her total responsibility as $1,999. (See second screenshot here.) So she got a new bill, but it didn’t change what she was asked to pay.


Always read the notes. This one is for an echocardiogram with Doppler, at an in-network provider. “I had my echocardiogram at my cardiologist’s office. However, I was billed a hospital facilities charge. I have insurance through my wife’s employer, her coworker paid $600 for the same procedure at her doctors office. I feel not only gouged for price but that the practice was deceptive and only minimum notice was given as to additional charges.” Also notice, the A32P note: “This amount reflects an additional medical expense being paid to the provider for this claim.” What does that actually mean? And the final note: “If this service was performed by an out-of-network provider without your knowledge this could be a surprise bill. Please see below information about surprise bills.” Apparently if it’s an in-network provider, it’s not a surprise bill?

We’ve said it before and we’ll say it again: A discount off a fancifully high charged rate is not a savings. But a bill that looks like this makes it seem that it is a savings. The really big number saying “Amount you saved” is the first thing you see, and the first thing you might take away: “Gosh, I’m glad my insurance company took care of that.” Essentially, that’s the insurance company’s writedown of the initial charge from the hospital to the insurer’s contract rate. Also, the man who input this bill into our database was certain that his insurance company had paid upwards of $10,000 for the echocardiogram in the second screenshot, too. As it happens, the insurer paid nothing; he paid the entire $1,176.61.
For a discussion of “anchoring” a person’s mind on a high price, see this blog post referring to seminal behavioral economics work by Daniel Kahneman and Amos Tversky.


Fairly clear here: A portion of the patient’s cost came from the deductible, and a portion from a 20 percent co-insurance charge. Co-insurance is figured on the member rate or allowable rate, less deductible. So: $3,482 allowed rate, less $437.81 deductible, equals $3044.19. Of that, plan pays 80 percent and patient pays 20 percent ($608.84).

Anesthesia cost figured courtesy of Fair Health, the New York health data giant created out of the Ingenix suit. A “Non Par Provider” does not participate in the health plan. So while this patient went to an in-network hospital, he had a non-participating anesthesiologist. The Fair Health data as used to establish this high cost for anesthesia during his surgery.

You would think that “total billed” – “contractual discount” = “Total allowed.” But no such thing. That’s only true in the first entry; the rest of he numbers seem random. The last entry, where the discount exceeds the charge, is a puzzler. The same surgery as the preceding bill.

A big string of zeroes. Same surgery as preceding two.

And more zeroes. Same surgery as preceding.

Final page of 4-page bill for this one surgery. Notice that nothing is ever added up as a total.


This person was absolutely sure that the insurance company had paid $857.49 + $352.23 = $1,209.72, though the bigger sum was clearly labeled “payment” and the “contractual adjustment” was labeled as such.
Is it a payment or an adjustment? Wait, it’s both! This bill clearly identifies the sum of $722.13 as both a payment and an adjustment. The vertical “payments” column is quite clear. Just as clearly, there was no payment at all, judging from the horizontal selection.

Check out the notes: We’re not paying this! Hospital bill for a hernia operation in Arizona.

Second bill for the above hernia operation, this one for the anesthesia.

Third bill for the hernia operation, this one for the surgeon.

Three stars for clarity. Charge is for “58110 Bx done w/colposcopy add-on.” But the code for the procedure is nowhere visible on the bill. Other points: Plan discount, amount allowed, plan paid, fairly clear. Also what’s deductible, copay, co-insurance. We’re confused by the coinsurance, though: Of the second surgery charge, $18.86 is deductible and, coinsurance is $11.33? We’d have to see the plan document, deductible status (how much was spent) and then the coinsurance language — do they pay X percent of the remainder after the deductible is spent? Anyway, this is a pretty clear EOB — aside from the fact that they don’t say what this is all about in anything like standard medical coding language. San Francisco Gynecology, San Francisco.

Very clear: Charged price, discount and payment are easy to understand. Why the system works this way is less clear, but at least some things are obvious — if you know what “Blue Cross discount” and “allowed amount” actually mean.

Multiple duplicate charges. This seems designed to confuse: All the duplicate charges in the red boxes make it clear that the total is the total only of some of the charges, the ones with *** notations. What possible value comes from listing them twice?

Payment clear, LOA seems to be the write-down. This was for treatment of an ectopic pregnancy. Fairly clear.

Confusing: No information on what kind of tests these were.

We’re just not going to pay. That is all. This is an EOB for removing impacted ear wax. Note that there is a “provider discount” and then “excluded charges,” with the notes explaining first that the insurer threw out $20.05 because this is “maximum benefit paid per schedule” and then threw out $19.62 because it is “not a listed policy benefit.” Also catch the wording under the triple asterisks: “The company does not waive and specifically reserves its right to assert and rely upon any/all reasons for which coverage for this claim may not be available under the terms of your coverage.” What language is this? What does it mean?

That’s a pricey doctor visit, at Swedish Cherry Hill in Seattle. “Doctor actually spent 10-15 minutes with me. And the problem was light pain in wrist.”

Again, the insurer paid nothing. This is such a common occurrence, it seems almost routine: conflating the payment and adjustment to make it seem that the insurer paid. Of course, the insurer paid nothing. In this case, at least you can see it; in other cases, there is no clarifying breakdown at all. The person who received the bill felt certain that the insurer had paid.

Sometimes it looks as if chimpanzees are typing in a random string of numbers. Note here that the “contractual discount” either equals the total billed, or is greater than the charge of $2. And in the final entry, the total billed, minus contractual discount, should be the total allowed. Nope. This was an emergency hospitalization, so the “bill does not match authorization” note makes little sense.

What are all these $1 charges for? They clearly perform some function from the provider (a hospital) and the insurer, but it’s a complete mystery otherwise. “Service is Never Pay” doesn’t actually tell us much. The final one, a charge of $1 with a contractual discount of $842, is a real head-scratcher.

At least adjustments and payments are separated out. What’s less clear: The bill of $1,079.00 results in total payments of $109.65, almost a 10x markup. Note how confusing it is that the charges all wind up in the “you pay” column — and then the adjustments and insurance payment are removed, insuring confusion. Notice too that it’s impossible to determine what the insurer paid for any test. And why are the Vitamin B and Vitamin D tests so expensive? In fact, at a second glance, all of these charged prices are high. These are routine tests from an annual physical.

That’s one expensive colonoscopy.

Colonoscopy charges include “sterile supply.” Wonder if other colonoscopies use nonsterile supplies? Also, what’s with the more than $700 in lab charges?

How much does dotarem (gadoterate meglumine) cost? It is a contrast agent that is injected into a body part for the “With contrast” type of MRI — to assess the status of the site if there has been surgery or some other disruption.

Never seen this: Writedown is “provider responsibility amount.” This is a mammogram. It would confuse anyone.

What it looks like when you have dense breast tissue. The insurer didn’t pay a penny. She has these screenings every six months on doctor’s orders.

No explanation of why a charge of $400 becomes balance due of $280, while a charge of $250 becomes balance due of $246.26. This is a follow-up mammogram after an initial free screening one.

Again, the “adjustment” is interpreted by the patient as the insurer’s payment. People just don’t see — or don’t correctly decipher — the fact that the Payment column is empty while the Adjustment column has a number in it. This was a brain MRI with and without contrast — and please note that the charge for the contrast material went directly to the patient. The patient also could not identify the procedure — there’s no CPT code, and he identified it as “other,” not the brain MRI without contrast described here.

The insurer paid nothing. Once again, the patient believed that the insurer paid $17.547. This was a hospital experience for “Reduce testis tortion.”

There’s information in the footnotes. The $292.95 is not what the insurer paid, but rather the insurer’s discount. See footnote 066. The patient construed this as a payment from the insurer, once again thanks to misleading EOB design.

Patient with high deductible pays a ton for routine blood tests. His portion: $1,474.92. Of course the EOB does not identify which test was which. The hospital estimate, the patient said, was “between $24.00 and $1,500.00.” He never received an itemized bill from the hospital, only this from the insurer. And his hospital chart shows these tests: Folate, Vitamin D Total (25OH), Vitamin B-12, Sed Rate, Hemoglobin A1C, Comprehensive Metabolic Panel, TSH, CBC with Auto Diff, Serum Protein Electrophoresis and Immunofixation. He added: “Healthcare Blue Book estimated each and every test uploaded to my UNC Chart at a cost below $50.00 for our zip code area.”

An appendectomy: Insurer inflates hospital’s bill. “Somehow my insurance adjusted the amount owed to be almost double what the hospital billed. So instead of owing my 30% on the amount billed $2397 I now owe $4224.30. “

Bill for an MRI reveals two things: Medicare is involved, and that’s a lot for Medicare to pay. The person who sent it in was utterly convinced that his insurer, a Medicare Advantage plan, had paid $2,334.02 — the combination of “Medicare Payments/Adj.” and “Insurance payments/Adj.” Problem is, Medicare’s rate in this area, Maine, is $461. What happened? We’ll find out. Also please note 3% prompt-pay discount.

CPAP machine. The comment: “The original cost of the Philips Respironics DreamStation CPAP machine was $3335.00. Cigna negotiated it to the 1667.50. However, the same machine with all its components can be purchased from Walmart for $499. I was never told what the machine would cost ahead of time. When after two weeks I was unhappy with using it, the Sleep Disorders Center of Connecticut people told me they would not buy it back, —that I could only donate it back. Instead, I’m trying to sell it on Craigslist. “

Emergency room visit for kidney stones. She thought the insurer paid $20,529.0, but of course it did not. She said “Was seen for 4 hours in emergency room related to a kidney stone. Doctor spend total of 15 minutes with me over the course of that 4 hour period. Had an x-ray and several shots. They lied about number of shots. I only had 2 shots of morphine and one fentanyl. They charged me for WAY more shots than I had been given. Crazy how much this place charges. THANK GOD I had insurance.”

Once again, the design is misleading. The payment from the insurer is clearly $0.00. Adjustments labeled as HADJ COMMERCIAL CONTRACTUAL. Patient read this as a payment from the insurer of $763.76. The copay for an emergency room visit is $500, and he was liable for $1,001.24 on top of that.

What the heck are “drugs requiring detailed coding”? We have no idea and neither did she, but they were billed at $12,909.05.

Billed for two colonoscopies at the same time. One code is 45385, one 45380. It sometimes happens. Here’s an explanation from a site that services medical coders. Obviously the insurance company wasn’t having any of it — they had an “adjustment” that wiped away one.

No clue what any of these numbers mean. But they’re big! This was an emergency room visit for a head injury overnight (which is why there are two dates of service).

Coinsurance of 20 percent of allowed rate. This was a cystoscopy and lithotripsy for kidney stones. The payments and adjustments are clearly broken out. The patient’s co-insurance was $599, which seems to be 20 percent of the “allowed amount” for the first procedure, $2,997.60.

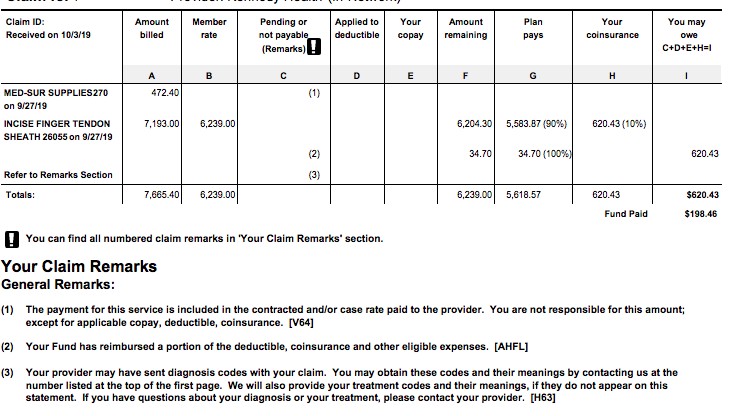
Co-insurance of 10 percent. This bill, for finger tendon surgery, shows that the plan paid 90 percent of the allowable $6,239, with the patient paying both $34.70 as part of her deductible and also co-insurance of $620.43, which the bill says is 10 percent of the allowable rate. But shouldn’t her 10 percent have been $623.90?
Physical therapy: $60 per ice pack. She said “Ice pack! $60 each time my 13 year old daughter used an ice pack at her physical therapy appointments for her sprained ankle. We were not given the ice pack to keep. It went back into their freezer. She used it for 10 minutes. Not ice therapy, just $60 for them to hand her an ice pack! The rest of the bill is infuriating. I asked for up front pricing and was told “we can’t give you that. There’s no way of knowing what it is”’

Emergency room visit for suspected heart attack. Insurer paid only one of the three “pharmacy” charges and ignored the rest.

Three hours: $223,404. Part of a bill for an emergency visit. She said: “The above charges are for the facility only. The doctors charges were 3456.00. The procedure, they went through my groin, shot dye in my left leg, and found a blood clot behind my knee, and blasted it and sucked it out. They gave me a valium, and a little gas. I was there maybe 3 hours. “

Befuddling. So many charges for “Hospital Misc.” And the helpful “Laboratory.” But what do any of these really mean? This was surgery for insertion of a pacemaker.



Sometimes it seems as if chimpanzees are typing in random numbers, Chapter 486. Surgery for a bone spur in the shoulder. The surgeon charged $8,100, the insurer allowed $147.73, of which the insurer paid $110.81 and the patient $36.92. Where do these charge numbers even come from?

How much does childbirth cost? This was a routine vaginal delivery. The first charge, $5,300, was for antepartum care, delivery and postpartum care. The bill conflates payment and adjustment, assigning them a total of $2,862.62, with patient responsibility of $2,418.38. The total hospital bill was $44,037, of which the insurer paid $8.098.20 and wrote down by $35,039. The patient was left with $899.80 for the hospital part. The baby got a separate bill.

Emergency appendectomy. Look at those writedowns!

Emergency room visit for cut finger. This is a Kaiser hospital, and a Kaiser insured person. So the $1,722.40 was a markup from Kaiser that was then marked down by Kaiser, leaving the actual cost, $365, paid by the patient.

Same bill from doctor and insurer. Note that insurer (on top) describes writedown as “Discount” while doctor (on bottom) describes writedown as “Adjustment.” Insurer paid nothing, but patient was certain that it had paid the entire amount of the discount. Laryngoscopy and endoscopy charges were accompanied by a bill for $655 for a “new patient visit,” which as written down to $324.14.


How much does a hip replacement cost, $95,459.83 or $77,967? Or $63,604? A friend had a hip replacement recently, and she sent over her bill. What’s interesting to us is, among other things, the Hospital for Special Surgery bill and the Cigna bill don’t add up.
Cigna reports that it was billed $95,459.83; HSS reports that it billed $63,604.00, absent physical therapy that was billed to Cigna.
Cigna’s “payments and adjustments” were $88,585.53, per HSS.
On its bill, Cigna reported that its payments were $77,967.86, and discounts were $17,468.50. Some of this does add up: That totals $95,436.36. My friend paid $23.47, according to the bill, as a copay for a semi-private ward.
It’s not clear that any of this is apples to apples.
The bills don’t match up in any sense, and one wonders about Cigna’s mysterious “ancillary charge” of $25,005.00, plus “service charges” of $512.80 and $6,338.03.
One of the Cigna “supplies” lines is $34,937.00; that seems to be the total of the four C1776 items and one C1713 — this is the actual hip implant and the screw, which add up to $34,937. Cigna paid exactly half, $17,468.50.
It seems everything else it paid in full, with no discount. We find this very unusual: insurers almost always discount off the charged price.
The first document is the Cigna explanation of benefits. Below that is the three-page itemized bill from HSS.






